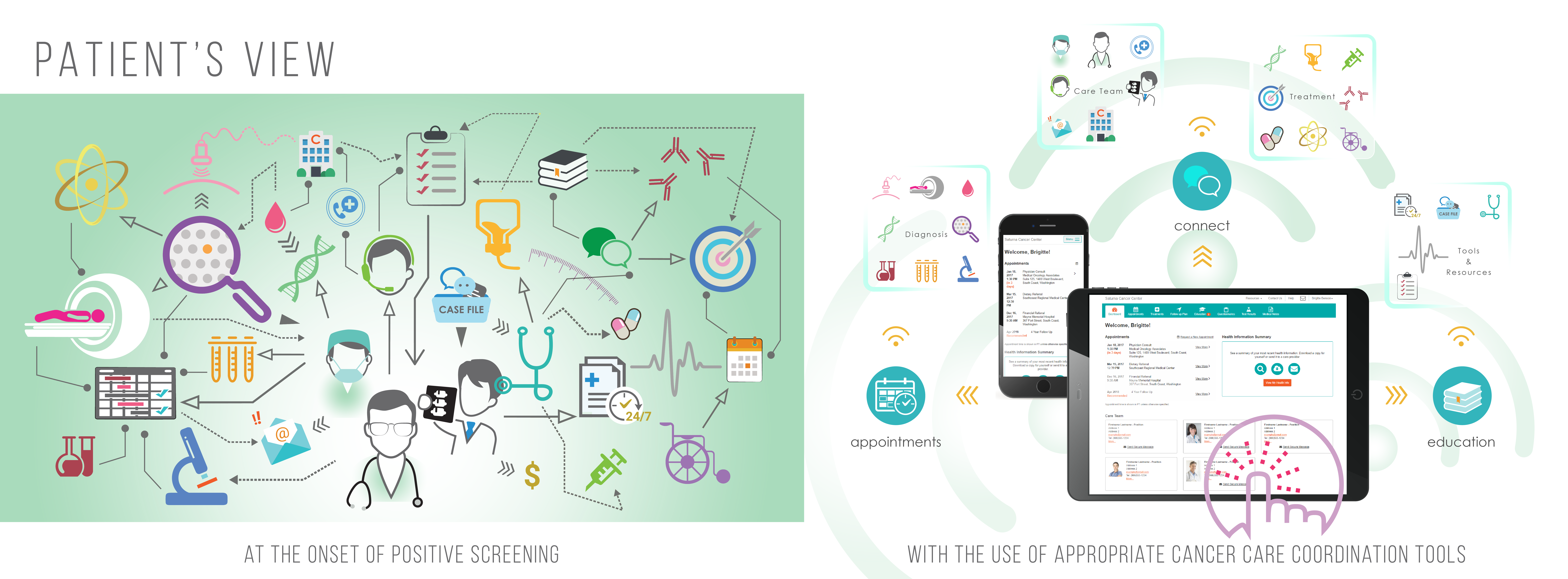
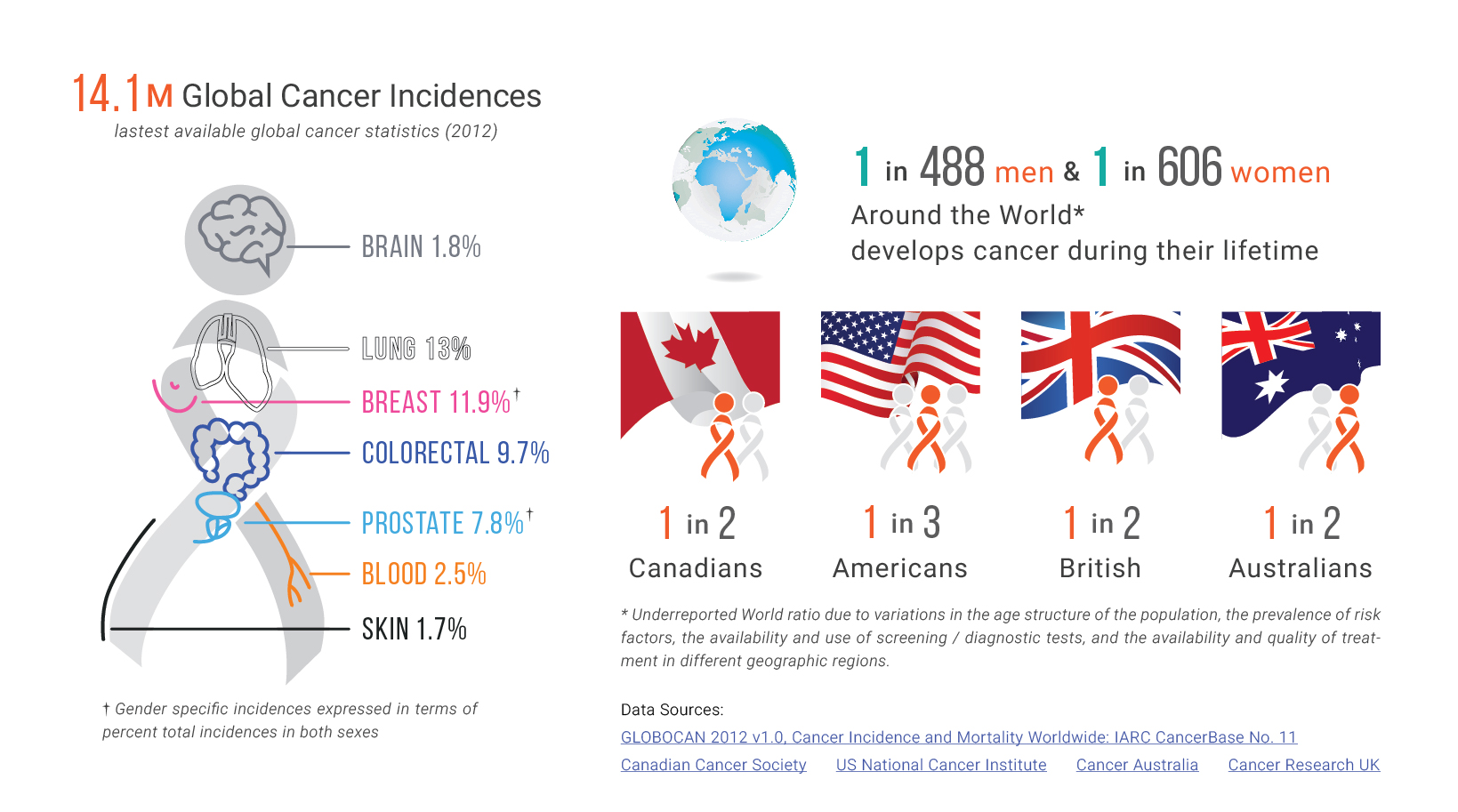
Cancer Care: From screening positive to diagnosis, and oncology team connection
Cancer screening procedures strive for effective early detection. In order to screen large numbers of at risk individuals, screening practices need to be simple, cheap and efficient. Diagnostic tests are used to determine the presence or absence of cancer. Symptomatic individuals, or individuals with positive cancer screening results, go through potentially invasive and expensive diagnostic procedures to establish the presence of a tumor.
As the cancer journey is complex and convoluted, the patient needs to meet with health professionals with different skill sets to facilitate the process. An oncologist oversees a patient’s care from diagnosis and throughout the course of treatment. Patients consult with their general practitioner and, at times in combination with, health insurance providers to be referred to the most appropriate oncologist. Databases, such as the American Society of Clinical Oncology (ASCO) [1], also provide open access lists.
Within the United States, approximately one third of patients aged 0 – 64 years (a population of approximately over 90 million) are referred to a specialist by their primary care physician [2]. A well-coordinated referral system needs to be established to accommodate this high frequency of referrals, in addition to connecting primary and specialty care.
All members of the oncology care team (oncologists, general practitioners, radiologists, nurse navigators, patient coordinators, registered dietitians, etc.) play an integral role in enhancing the quality of care received. The care provided encompasses diverse aspects of health services. In addition to appropriate care that is timely and appropriate, other elements of cancer care include psychosocial assessment, suitable and timely referral, and individualized treatment that considers each patient’s needs and preferences. A multidisciplinary team is needed to address these tasks, which may create complexities to care coordination in both hospital and community settings. Challenges include recognizing health professional roles and responsibilities, communication between the care team and with the patient, managing scarce resources, and transitioning patients through care.
Digital technologies have aimed to address these challenges [3]. These include:
-
Electronic portals
-
Electronic Health Records (EHRs)
-
Patient reported outcomes measures
-
Patient-centered education
They are utilized to enable collaborative care coordination systems. Patient experience and outcome is enhanced when implementation of optimal technologies are coupled with proper training and support for patients and the care team.
Recent evidence-based research has proven that improving quality of care through enhanced communication and a well-coordinated system is advantageous for the patient, the medical team, and healthcare system. Researchers have embarked on a series of studies aimed at identifying quality measures. Two examples of these cover:
1. The impact of EHRs and oncology EMR tools used by multidisciplinary teams in GP-oncologist communication and facilitation of cancer care. [4]
2. Use of IT-enabled measurements and patient reported outcomes by patients and the care team to enhance patient-centered care (allowing for a seamless incorporation of patient perspectives into cancer care practices). [5]
As a patient moves through from screening and diagnostics to workup, treatment plan, and the care planning stages – clear communication, education tools, and access improve patient engagement.
In our next article, we will take a closer look at different ways of engaging patients and their caregivers (e.g. patient portals, patient reported outcomes, and patient-centred education), and how they can ultimately improve the quality of health outcomes.
Main resources: https://www.ncbi.nlm.nih.gov/books/NBK223387/
Written by Dorri Mahdaviani , who holds a Masters of Public Health (MPH) from the University of British Columbia (UBC). Her academic and professional interests include the areas of chronic illnesses, health care systems and childhood health and development.
Infographics and Design by Ann Wong, who holds a PhD in Biochemistry and Molecular Biology from the Faculty of Medicine at the University of British Columbia (UBC), Canada. She is an author of over 10 SCI publications, having taught at UBC and the Peking University Health Science Center (PUHSC) in Beijing.